Respiratory System - PowerPoint PPT Presentation
Title:
Respiratory System
Description:
The respiratory system regulates blood p H by regulating plasma carbon dioxide levels 23-* Respiratory Areas in the Brainstem Medullary respiratory center Dorsal ... – PowerPoint PPT presentation
Number of Views:231
Avg rating:3.0/5.0
Title: Respiratory System
1
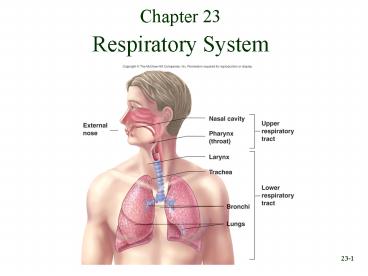
Chapter 23
- Respiratory System
2
Respiration
- Ventilation Movement of air into and out of
lungs - External respiration Gas exchange between air in
lungs and blood - Transport of oxygen and carbon dioxide in the
blood - Internal respiration Gas exchange between the
blood and tissues
3
Respiratory System Functions
- Gas exchange Oxygen enters blood and carbon
dioxide leaves - Regulation of blood pH Altered by changing blood
carbon dioxide levels (increase CO2 decrease
pH) - Voice production Movement of air past vocal
folds makes sound and speech - Olfaction Smell occurs when airborne molecules
are drawn into nasal cavity - Protection Against microorganisms by preventing
entry and removing them from respiratory surfaces.
4
Respiratory System Divisions
- Upper tract nose, pharynx and associated
structures - Lower tract larynx, trachea, bronchi, lungs and
the tubing within the lungs
5
Nose (Nasus) and Nasal Cavities
- External nose (visible part includes hyaline
cartilage plates nasal bones ) - Nasal cavity
- From nares (nostrils) to choanae (openings into
the pharynx) - Vestibule just inside nares lined with
stratified squamous epithelium continuous with
skin - Hard palate floor of nasal cavity separates
nasal cavity from oral cavity covered by mucous
membrane - Nasal septum partition dividing cavity. Anterior
cartilage posterior vomer and perpendicular
plate of ethmoid (divides nasal cavity into right
left parts) - Choanae bony ridges on lateral walls with
meatuses (passageways) between. Openings to
paranasal sinuses and to nasolacrimal duct
6
Functions of Nasal Cavity
- Passageway for air (open even if mouth full of
food) - Cleans the air vestibule lined with hair this
traps particles / mucous membrane consists of
pseudostratified ciliated columnar epithelium
with goblet cells (mucus) - Humidifies( moisture from mucous membranes from
excess tears that drains into nasal cavity
through nasolacrimal duct), warms air ( warm
blood flowing through mucous membranes - this
prevents damage to respiratory passages caused by
cold air) - Smell superior part of nasal cavity consists of
olfactory epithelium (sensory receptors) - Along with paranasal sinuses are resonating
chambers for speech
7
Pharynx
- Common opening for digestive and respiratory
systems (connected to respiratory at larynx to
digestive at esophagus) - Three regions
- Nasopharynx
- a. Pseudostratified columnar epithelium with
goblet cells. - b. Mucous and debris from nasal cavity is
swallowed. - c. Openings of Eustachian (auditory) tubes air
that passes through them to equalize air pressure
between atmosphere middle ear. - d. Floor is soft palate (separates nasopharynx
from oropharynx), uvula is posterior extension of
the soft palate prevents swallowed materials
from entering nasopharynx nasal cavity
- Oropharynx shared with digestive system (extends
from soft palate to epiglottis). Lined with moist
stratified squamous epithelium air, food,
drink passes through. - Laryngopharynx epiglottis to esophagus. Lined
with moist stratified squamous epithelium food
drink pass through here to esophagus (very
little air passes / - too much air gas)
8
Larynx
9
Larynx - base of tongue to trachea / passageway
for air
- Unpaired cartilages
- Thyroid largest, Adams apple
- Cricoid most inferior, base of larynx (other
cartilages rest here) - Epiglottis attached to thyroid and has a flap
near base of tongue. Elastic rather than hyaline
cartilage - Paired
- Arytenoids attached to cricoid
- Corniculate attached to arytenoids
- Cuneiform contained in mucous membrane
- Ligaments extend from arytenoids to thyroid
cartilage - Vestibular folds or false vocal folds
- True vocal cords or vocal folds sound
production. Opening between is glottis -
laryngitis is an inflammation of mucosal
epithelium of vocal folds
10
Functions of Larynx
- Maintain an open passageway for air movement
thyroid and cricoid cartilages - Epiglottis and vestibular folds prevent swallowed
material from moving into larynx during
swallowing, epiglottis covers the opening of
larynx so, food liquid slide over epiglottis
toward esophagus. Also, closure of vestibular
folds can also prevent the passage of air----when
person holds breath. - Vocal folds are primary source of sound
production. Greater the amplitude of vibration,
louder the sound (force of air moving past vocal
cords determines amplitude). - Frequency of
vibration determines pitch. Also, length of
vibrating segments of vocal folds
affect-------ex when only anterior parts of
folds vibrate, higher pitched tones are produced
when longer sections of vibrate, lower tones
result. - - Arytenoid cartilages and skeletal muscles
determine length of vocal folds and also
abduct the folds when not speaking (only
breathing) to pull them out of the way making
glottis larger (allows greater movement of air). - The pseudostratified ciliated columnar epithelium
(lines larynx) traps debris, preventing their
entry into the lower respiratory tract.
11
Vocal Folds
12
Trachea - windpipe
- Membranous tube of dense regular connective
tissue and smooth muscle supported by 15-20
hyaline cartilage C-shaped rings (protects
maintains open passageway for air) . Posterior
surface is devoid of cartilage contains elastic
ligamentous membrane and bundles of smooth muscle
called the trachealis. - Contracts during coughing-----this causes air
to move more rapidly through trachea, which helps
expel mucus foreign
objects. - Inner lining pseudostratified ciliated columnar
epithelium with goblet cells. Mucus traps debris,
cilia push it superiorly toward larynx and
pharynx. - Divides to form
- Left and right primary bronchi (each extends to a
lung) - Carina cartilage at bifurcation (forms ridge).
Membrane of carina especially sensitive to
irritation and inhaled objects initiate the cough
reflex
13
Tracheobronchial Tree and Conducting Zone
- Trachea to terminal bronchioles which is ciliated
for removal of debris. - Trachea divides into two primary bronchi. (right
is larger in diameter more in line with trachea
than left) - Primary bronchi divide into secondary (lobar)
bronchi (one/lobe) which then divide into
tertiary (segmental) bronchi. - Bronchopulmonary segments defined by tertiary
bronchi.
- Tertiary bronchi further subdivide into smaller
and smaller bronchi then into
bronchioles (less than 1 mm in diameter), then
finally into terminal bronchioles. - Cartilage holds tube system open smooth muscle
controls tube diameter----- - ex during exercise, diameter increases,
decreases resistance to airflow, increases volume
of air moved - during asthma attack, diameter decreases,
increases resistance to airflow, decreases volume
of air flow - As tubes become smaller, amount of cartilage
decreases, amount of smooth muscle
increases------ex terminal bronchioles have no
cartilage only have smooth muscle.
14
Respiratory Zone Respiratory Bronchioles to
Alveoli
- Respiratory zone site for gas exchange
- Respiratory bronchioles branch from terminal
bronchioles. Respiratory bronchioles have very
few alveoli (small, air filled chambers where gas
exchange between air blood takes place). Give
rise to alveolar ducts which have more alveoli.
Alveolar ducts end as alveolar sacs that have 2
or 3 alveoli at their terminus. - Tissue surrounding alveoli contains elastic
fibers (alveoli expand during inspiration
recoil during expiration) - No cilia, but debris removed by macrophages.
Macrophages then move into nearby lymphatics or
into terminal bronchioles.
15
The Respiratory Membrane
- Three types of cells in membrane.
- Type I pneumocytes. Thin squamous epithelial
cells, form 90 of surface of alveolus. Gas
exchange. - Type II pneumocytes. Round to cube-shaped
secretory cells. Produce surfactant (makes it
easier for alveoli to expand during inspiration).
- Dust cells (phagocytes)
- Layers of the respiratory membrane
- Thin layer of fluid lining the alveolus
- Alveolar epithelium (simple squamous epithelium
- Basement membrane of the alveolar epithelium
- Thin interstitial space
- Basement membrane of the capillary endothelium
- C apillary endothelium composed of simple
squamous epithelium - Tissue surrounding alveoli contains elastic
fibers that contribute to recoil.
16
Lungs
- Two lungs Principal organs of respiration
- Base sits on diaphragm, apex at the top, hilus
(hilum) on medial surface where bronchi and blood
vessels enter the lung. All the structures in
hilus called root of the lung. - Right lung three lobes. Lobes separated by
fissures (deep prominent) - Left lung Two lobes
- Right lung is larger heavier than left
- Divisions
- Lobes (supplied by secondary bronchi), each lobe
is subdivided into bronchopulmonary segments
(supplied by tertiary bronchi and separated from
one another by connective tissue partitions),
bronchopulmonary segments are subdivided into
lobules (supplied by bronchioles and separated by
incomplete partitions). - Note 9 bronchopulmonary segments present in left
lung 10 present right lung - Note Individual diseased bronchopulmonary
segments can be surgically removed, leaving the
rest of lung intact, because major blood
vessels bronchi do not cross connective tissue
partitions.
17
Thoracic Wall and Muscles of Respiration
18
Thoracic Wall
- Thoracic vertebrae, ribs, costal cartilages,
sternum and associated muscles - Thoracic cavity space enclosed by thoracic wall
and diaphragm - Diaphragm separates thoracic cavity from
abdominal cavity
19
Inspiration and Expiration
- Inspiration diaphragm, external intercostals,
pectoralis minor, scalenes - Diaphragm dome-shaped with base of dome attached
to inner circumference of inferior thoracic cage.
Central tendon top of dome which is a flat sheet
of connective tissue. - Quiet inspiration accounts for 2/3 of increase
in size of thoracic volume. Inferior movement of
central tendon and flattening of dome. Abdominal
muscles relax - Other muscles elevate ribs and costal cartilages
allow lateral rib movement - Expiration muscles that depress the ribs and
sternum such as the abdominal muscles and
internal intercostals. - Quiet expiration relaxation of diaphragm and
external intercostals with contraction of
abdominal muscles - Labored breathing all inspiratory muscles are
active and contract more forcefully. Expiration
is rapid
20
Effect of Rib and Sternum
21
Pleura
- Pleural cavity surrounds each lung and is formed
by the pleural membranes. Filled with pleural
fluid. - Visceral pleura adherent to lung. Simple
squamous epithelium, serous. - Parietal pleura adherent to internal thoracic
wall.
- Pleural fluid acts as a lubricant and helps hold
the two membranes close together (adhesion). - Mediastinum central region, contains contents of
thoracic cavity except for lungs.
22
Blood and Lymphatic Supply
- Two sources of blood to lungs Pulmonary
Bronchial - Pulmonary artery brings deoxygenated blood to
lungs from right side of heart to be oxygenated
in capillary beds that surround the alveoli.
Blood leaves via the pulmonary veins and returns
to the left side of the heart. - Bronchial arteries provide oxygenated systemic
blood to lung tissue. They arise from the aorta
run along the branching bronchi. Part of this now
deoxygenated blood exits through the bronchial
veins to the azygous (drains chest muscles) part
merges with blood of alveolar capillaries and
returns to left side of heart. - Blood going to left side of heart via pulmonary
veins carries primarily oxygenated blood, but
also some deoxygenated blood from the supply of
the walls of the conducting and respiratory zone. - Two lymphatic supplies superficial and deep
lymphatic vessels. Exit from hilus - Superficial drain superficial lung tissue and
visceral pleura - Deep drain bronchi and associated C.T.
- No lymphatics drain alveoli
- Phagocytic cells within lungs phagocytize carbon
particles other debris from inspired air move
them to lymphatic vessels - Older people smokers lungs appear gray to black
because accumulation of these particles - Cancer cells from lungs can spread to other parts
of body through lymphatic vessels.
23
Ventilation
- Movement of air into and out of lungs
- Air moves from area of higher pressure to area of
lower pressure (requires a pressure gradient) - If barometric pressure (atmospheric pressure) is
greater than alveolar pressure, then air flows
into the alveoli. - Boyles Law P k/V, where P gas pressure,
- V volume, k constant at a given temperature
- If diaphragm contracts, then size of alveoli
increases. Remember P is inversely proportionate
to V so as V gets larger (when diaphragm
contracts), then P in alveoli gets smaller.
24
Alveolar Pressure Changes (Note Barometric air
pressure is always assigned a value of
zero)
25
Changing Alveolar Volume Lung Recoil( Lung
recoil changes in pleural pressure cause
changes in alveolar volume which results in
changes in pressure )
- Causes alveoli to collapse resulting from
- Elastic recoil elastic fibers in the alveolar
walls - Surface tension film of fluid lines the alveoli.
Where water interfaces with air, polar water
molecules have great attraction for each other
with a net pull in toward other water molecules.
Tends to make alveoli collapse. - (attracted molecules of fluid surface tension
draws alveoli to their smallest possible
dimension) - Surfactant Reduces tendency of lungs to collapse
by reducing surface tension. Produced by type II
pneumocytes. - Respiratory distress syndrome (hyaline membrane
disease). Common in infants with gestation age
of less than 7 months. Not enough surfactant
produced.
26
Pleural Pressure ( pressure in pleural cavity)
- Negative pressure can cause alveoli to expand
- Alveoli expand when pleural pressure is low
enough to overcome lung recoil - Pneumothorax is an opening between pleural cavity
and air that causes an increase of pleural
pressure (air gets into pleural cavity by an
opening in the thoracic wall or lung---------can
be caused by penetrating trauma ex knife,
bullet, broken rib or by non-penetrating trauma
ex blow to chest, medical procedure (inserting
catheter to withdraw pleural fluid), infections. - Causes part or all of the lung to collapse.
27
Normal Breathing Cycle (Inspiration pleural
pressure decreases alveolar volume increases
alveolar pressure decreases below barometric
pressure air flow into lungs.
28
Compliance
- Measure of the ease with which lungs and thorax
expand - The greater the compliance, the easier it is for
a change in pressure to cause expansion - A lower-than-normal compliance means the lungs
and thorax are harder to expand - Conditions that decrease compliance
- Pulmonary fibrosis deposition of inelastic
fibers in lung (emphysema) - Pulmonary edema (the alveoli fill with fluid
instead of air, preventing oxygen from
being absorbed into your bloodstream) - Respiratory distress syndrome
- Increased resistance to airflow caused by airway
obstruction (asthma, bronchitis, lung cancer) - Deformities of the thoracic wall (kyphosis
(hunchback), scoliosis)
29
Pulmonary Volumes and Capacities
- Spirometry measures volumes of air that move
into and out of respiratory system. Uses a
spirometer - Tidal volume amount of air inspired or expired
with each breath. At rest 500 mL - Inspiratory reserve volume amount that can be
inspired forcefully after inspiration of the
tidal volume (3000 mL at rest) - Expiratory reserve volume amount that can be
forcefully expired after expiration of the tidal
volume (100 mL at rest) - Residual volume volume still remaining in
respiratory passages and lungs after most
forceful expiration (1200 mL)
30
Pulmonary Capacities
- The sum of two or more pulmonary volumes
- Inspiratory capacity tidal volume plus
inspiratory reserve volume - Functional residual capacity expiratory reserve
volume plus residual volume - Vital capacity sum of inspiratory reserve
volume, tidal volume, and expiratory reserve
volume - Total lung capacity sum of inspiratory and
expiratory reserve volumes plus tidal volume and
residual volume. - Factors such as sex, age, body size, and
physical conditioning cause variations in
respiration capacities from one individual to
another. Ex males, younger people, thin people,
tall people, athletes------------have greater
vital capacities.
31
Spirometer, Lung Volumes, and Lung Capacities
32
Minute Ventilation and Alveolar Ventilation
- Minute ventilation total air moved into and out
of respiratory system each minute tidal volume X
respiratory rate - Respiratory rate (respiratory frequency) (f)
number of breaths taken per minute - Anatomic dead space formed by nasal cavity,
pharynx, larynx, trachea, bronchi, bronchioles,
and terminal bronchioles (part of respiratory
system where gas exchange does NOT take place) - Physiological dead space anatomic dead space
plus the volume of any alveoli in which gas
exchange is less than normal. (these are
nonfunctional alveoli--------few exist in healthy
individual) - Alveolar ventilation (VA) volume of air
available for gas exchange/minute VA f ( VT
VD) - VT tidal volume VD dead space
33
Physical Principles of Gas Exchange
- Partial pressure
- The pressure exerted by each type of gas in a
mixture - ex atmospheric pressure 760 mmHg
- (contains nitrogen 79 oxygen 21)
- Daltons law in a mixture of gases, the
percentage of each gas is proportionate to its
partial pressure - N2 79 79/100 0.79 ----?partial pressure
0.79 x 760 mmHg 600mmHg - partial pressure is denoted----? PN2
- Water vapor pressure pressure exerted by gaseous
water in a mixture of gases (water evaporated
into air) - Air in the respiratory system contains humidity
because of mucus lining system - Diffusion of gases through liquids (gas molecules
move from air into liquid, or from a liquid into
air, because of partial pressure gradient----ex
partial pressure of gas in the air is greater
than in the liquid, movement of gas molecules
into the liquid) - Henrys Law Concentration of a gas in a liquid
is determined by its partial pressure and its
solubility coefficient (solubility coefficient is
a measure of how easily the gas dissolves in the
liquid. Ex solubility coefficient for oxygen is
0.024 carbon dioxide is 0.57-----?CO2 is 24
times more soluble than O2 )
34
Physical Principles of Gas Exchange
- Diffusion of gases through the respiratory
membrane depends upon three things - Membrane thickness. The thicker, the lower the
diffusion rate (diseases can cause an increase in
thickness) - Diffusion coefficient of gas (measure of how
easily a gas diffuses through a liquid or
tissue). This takes into account the solubility
of the gases size of gas molecules (molecular
weight). CO2 is 20 times more diffusible than O2 - Surface area. Diseases like emphysema and lung
cancer reduce available surface area - Partial pressure differences. Gas moves from area
of higher partial pressure to area of lower
partial pressure. Normally, partial pressure of
oxygen is higher in alveoli than in blood.
Opposite is usually true for carbon dioxide
35
Relationship Between Alveolar Ventilation and
Pulmonary Capillary Perfusion
- Increased ventilation or increased pulmonary
capillary blood flow increases gas exchange - Shunted blood blood that is not completely
oxygenated - Physiologic shunt is deoxygenated blood returning
from lungs. Two sources - Blood returning from bronchi bronchioles
- Blood from capillaries around alveoli
- 1 - 2 of cardiac output makes up the
physiological shunt - Regional distribution of blood flow determined
primarily by gravity, but can also be determined
by alveolar PO2. - Low PO2 causes arterioles to constrict so that
blood is shunted to a region of the lung where
the alveoli are better ventilated. Ex when
bronchus becomes partially blocked - In other tissues of the body, low PO2 causes
arterioles to dilate to deliver more blood to the
tissues.
36
Oxygen and Carbon Dioxide Diffusion Gradients
- Oxygen
- Moves from alveoli into blood. Blood is almost
completely saturated with oxygen when it leaves
the capillary - PO2 in blood decreases because of mixing with
deoxygenated blood (because blood from pulmonary
capillaries mixes with deoxygenated blood from
bronchial veins) - Oxygen moves from tissue capillaries into the
tissues
- Carbon dioxide
- Moves from tissues into tissue capillaries
- Moves from pulmonary capillaries into the alveoli
37
Gas Exchange
38
Hemoglobin and Oxygen Transport
- Oxygen is transported by hemoglobin (98.5) and
is dissolved in plasma (1.5) - Oxygen-hemoglobin dissociation curve describes
the percentage of hemoglobin saturated with
oxygen at any given PO2 - Oxygen-hemoglobin dissociation curve at rest
shows that hemoglobin is almost completely
saturated when PO2 is 80 mm Hg or above. At
lower partial pressures, the hemoglobin releases
oxygen. - Thus, as tissues use more oxygen, hemoglobin
releases more oxygen - to those tissues.
39
Bohr Effect
- Effect of pH on oxygen-hemoglobin dissociation
curve as pH of blood declines, amount of oxygen
bound to hemoglobin at any given PO2 also
declines - Occurs because decreased pH yields increase in H
that combines with hemoglobin changing its
shape and oxygen cannot bind to hemoglobin
40
Effects of CO2 and Temperature
- Increase in PCO2 causes decrease in p H
- Carbonic anhydrase causes CO2 and water to
combine reversibly and form H2CO3 (carbonic
acid) which ionizes to H and HCO3-
(bicarbonate ion) - Increase temperature decreases tendency for
oxygen to remain bound to hemoglobin, so as
metabolism goes up, more oxygen is released to
the tissues.
41
Effect of BPG
- 2,3-bisphosphoglycerate (BPG) released by RBCs
as they break down glucose for energy - Binds to hemoglobin and increases release of
oxygen (reduces its affinity for oxygen) - Ex High altitudes decrease barometric
pressure partial pressure of oxygen in alveoli
decreased saturation of blood with oxygen in
pulmonary capillaries decreased less oxygen in
blood to be delivered to tissues - BPG helps increase oxygen delivery to tissues
because increased levels of BPG increase the
release of oxygen in tissues.
42
Shifting the Curve
43
Transport of Carbon Dioxide
- Carbon dioxide is transported as bicarbonate ions
(70) in combination with blood proteins (23
primarily alpha beta globin chains of
hemoglobin) and in solution with plasma (7) - Hemoglobin that has released oxygen binds more
readily to carbon dioxide than hemoglobin that
has oxygen bound to it ( Haldane effect) - In tissue capillaries, carbon dioxide combines
with water inside RBCs to form carbonic acid
which dissociates to form bicarbonate ions and
hydrogen ions
44
Carbon Dioxide Transport and Chloride Movement
- (a) Tissue capillaries as C O2 enters red blood
cells, reacts with water to form bicarbonate and
hydrogen ions. C hloride ions enter the RB C
and bicarbonate ions leave chloride shift. H
ydrogen ions combine with hemoglobin. (pH of RBC
does not decrease bec. hemoglobin is a buffer )
Lowering the concentration of bicarbonate and
hydrogen ions inside red blood cells promotes the
conversion of C O2 to bicarbonate ion. - (b) Pulmonary capillaries C O2 leaves red blood
cells, resulting in the formation of additional
C O2 from carbonic acid. The bicarbonate ions are
exchanged for chloride ions, and the hydrogen
ions are released from hemoglobin. - Increased plasma carbon dioxide lowers blood p H.
The respiratory system regulates blood p H by
regulating plasma carbon dioxide levels
45
Respiratory Areas in the Brainstem
- Medullary respiratory center
- Dorsal groups stimulate the diaphragm
- Ventral groups stimulate the intercostal and
abdominal muscles - This section is especially sensitive during
infancy, and the neurons can be destroyed if the
infant is dropped and/or shaken violently. The
result can be death due to "shaken baby syndrome - Pontine (pneumotaxic) respiratory group
- Involved with switching between inspiration and
expiration (fine tunes the breathing
pattern-----there is a connection with medullary
resp. center but precise function unknown)
46
Rhythmic Ventilation
- Starting inspiration
- Medullary respiratory center neurons are
continuously active - Center receives stimulation from receptors (that
monitor blood gas levels) and simulation from
parts of brain concerned with voluntary
respiratory movements and emotion - Combined input from all sources causes action
potentials to stimulate respiratory muscles - Increasing inspiration
- More and more neurons are activated (to stimulate
respiratory muscles) - Stopping inspiration
- Neurons stimulating the muscles of respiration
also stimulate the neurons in the medullary
respiratory center that are responsible stopping
inspiration. They also receive input from
pontine group and stretch receptors in lungs.
Inhibitory neurons activated and relaxation of
respiratory muscles results in expiration. - Note although the medullary neurons establish
the basic rate depth of breathing, their
activities can be influenced by input from other
parts of the brain by input from peripherally
located receptors.
47
Rhythmic Ventilation
- Chemical control
- Carbon dioxide is major regulator, but indirectly
through p H change - Increase or decrease in pH can stimulate
chemo-sensitive area, causing a greater rate and
depth of respiration - Oxygen levels in blood affect respiration when a
50 or greater decrease from normal levels exists - CO2.
- Hypercapnia too much CO2
- Hypocapnia lower than normal CO2
- Apnea. Cessation of breathing. Can be conscious
decision, but eventually PCO2 levels increase to
point that respiratory center overrides - Hyperventilation. Causes decrease in blood PCO2
level, which causes respiratory alkalosis (high
blood pH). Fainting, leads to changes in the
nervous system fires and leads to the paresthesia
(pins needles) - Cerebral (cerebral cortex)and limbic system.
Respiration can be voluntarily controlled and
modified by emotions (ex strong emotions can
cause hyperventilation or produce the sobs
gasps of crying)
48
Modifying Respiration
49
Chemical Control of Ventilation
- Chemoreceptors specialized neurons that respond
to changes in chemicals in solution - Central chemoreceptors chemosensitive area of
the medulla oblongata connected to respiratory
center - Peripheral chemoreceptors carotid and aortic
bodies. Connected to respiratory center by
cranial nerves IX and X (9 10) - Effect of pH chemosensitive area of medulla
oblongata and carotid and aortic bodies respond
to blood pH changes - Chemosensitive areas respond indirectly through
changes in carbon dioxide - Carotid and aortic bodies respond directly to p H
changes
50
Chemical Control of Ventilation
- Effect of carbon dioxide small change in carbon
dioxide in blood triggers a large increase in
rate and depth of respiration - - ex an increase PCO2 of 5 mm Hg causes an
increase in ventilation of 100. - Hypercapnia greater-than-normal amount of carbon
dioxide - Hypocapnia lower-than-normal amount of carbon
dioxide - Chemosensitive area in medulla oblongata is more
important for regulation of PCO2 and pH than the
carotid aortic bodies (responsible for 15 -
20 of response) - During intense exercise, carotid aortic bodies
respond more rapidly to changes in blood pH than
does the chemosensitive area of medulla
51
Chemical Control of Ventilation
- Effect of oxygen carotid and aortic body
chemoreceptors respond to decreased PO2 by
increased stimulation of respiratory center to
keep it active despite decreasing oxygen levels
(50 or greater decrease----------bec. of
oxygen-hemoglobin dissociation curve-------at any
PO2 above 80 mm Hg nearly all of hemoglobin is
saturated with oxygen) - Hypoxia decrease in oxygen levels below normal
values
52
Regulation of Blood pH and Gases
53
Hering-Breuer Reflex
- Limits the degree of inspiration and prevents
overinflation of the lungs - Depends on stretch receptors in the walls of
bronchi bronchioles of the lung. - It is an inhibitory influence on the respiratory
center results in expiration. (as expiration
proceeds, stretch receptors no longer stimulated)
- Infants
- Reflex plays a role in regulating basic rhythm of
breathing and preventing overinflation of lungs - Adults
- Reflex important only when tidal volume large as
in exercise
54
Effect of Exercise on Ventilation
- Ventilation increases abruptly
- At onset of exercise
- Movement of limbs has strong influence (body
movements stimulate proprioceptors in joints of
the limbs) - Learned component (after a period of training,
the brain learns to match ventilation with the
intensity of exercise) - Ventilation increases gradually
- After immediate increase, gradual increase occurs
(4-6 minutes it levels off) - Anaerobic threshold highest level of exercise
without causing significant change in blood pH.
If exercise intensity is high enough to exceeded
anaerobic threshold, lactic acid produced by
skeletal muscles
55
Other Modifications of Ventilation
- Activation of touch, thermal and pain receptors
affect respiratory center - Sneeze reflex (initiated by irritants in the
nasal cavity), cough reflex (initiated by
irritants in the lungs) - Increase in body temperature yields increase in
ventilation
56
Respiratory Adaptations to Exercise
- Athletic training
- Vital capacity increases slightly residual
volume decreases slightly - At maximal exercise, tidal volume and minute
ventilation increases - Gas exchange between alveoli and blood increases
at maximal exercise - Alveolar ventilation increases
- Increased cardiovascular efficiency leads to
greater blood flow through the lungs
57
Effects of Aging
- Vital capacity and maximum minute ventilation
decrease (these changes are related to weakening
of respiratory muscles decreased compliance of
thoracic cage caused by stiffening of cartilage
ribs) - Residual volume and dead space increase
- Ability to remove mucus from respiratory
passageways decreases - Gas exchange across respiratory membrane is
reduced