Bariatric Surgery PowerPoint PPT Presentation
1 / 41
Title: Bariatric Surgery
1
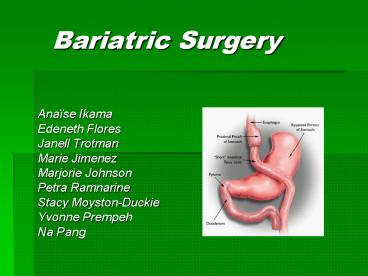
Bariatric Surgery
- Anaïse Ikama
- Edeneth Flores
- Janell Trotman
- Marie Jimenez
- Marjorie Johnson
- Petra Ramnarine
- Stacy Moyston-Duckie
- Yvonne Prempeh
- Na Pang
2
What is Bariatric Surgery
- by
- Yvonne Prempeh
3
What is bariatric surgery?
- Bariatric surgery is the term for operations to
help promote weight loss. - There are three types of bariatric surgery
- LAP- BAND system,
- Vertical Banded
- Gastroplasty(VBD), Roux-en-Y Gastric Bypass
4
LAP BAND SYSTEM
- An adjustable silicone elastic band is placed
around the upper part of the stomach creating a
small pouch and restricting the passage of food
5
VERTICAL BANDED GASTROPLASTY (VBG)
- VBG is a purely restrictive procedure in which
the upper stomach is stapled and divided, forming
a small pouch that reduces the size of the
stomach and the amount of food the stomach can
hold
6
ROUX-EN-Y GASTRIC BYPASS
- Roux-en-Y Gastric Bypass is the most frequently
performed weight loss procedure in the United
States - During this surgery, the upper stomach is stapled
creating a small pouch that is completely divided
from the remainder of the stomach
7
Requirements for Bariatric surgery
by Petra Ramnarine
8
Criteria before surgery
- BMI of 40
- 80 - 100lbs overweight
- Diabetes, heart disease or severe apnea
- Related physical problems that significantly
employment, physical mobility or physical
function
9
Criteria for insurance companies
- Obtaining approval can take up to 4 weeks from
insurance company - Pt will be responsible for out of pocket fees as
outlined in policies
10
Nutrition Diet plan for Bariatric Surgery
by Janell Trotman
11
Nutrition
- Patient have to follow a strict diet before and
after bariatric surgery. - Patient must have a nutritional consultation.
12
Pre-Post Operative Nutrition
- Clients are started on a puree or liquid diet 2
weeks before surgery. - Most of the caloric intake should contain mostly
of protein. - Caffeine, soda, alcoholic and beverages that
contain sugar should be avoided.
13
Food Restriction
- It is important to chew food thoroughly and slow
- It is important wait 2-3 minutes after
swallowing before putting the next bite of food
in your mouth. - Dont drink fluids while eating
14
Food Restrictions
- Avoid food high in fat and have no nutritional
value.
15
Food Restriction
- Avoid alcohol
- Avoid food high in sugar
- Limit snacking between meals
16
Pre-operative Nursing Care
- By Marjorie Johnson
17
Pre-operative Nursing Care
- There are always risks with surgery, however as
health care providers, we can follow steps to
minimize these risks by performing physical and
psychosocial assessment of the patient. The
psychosocial assessment is obtained to evaluate
the patients mood, self-esteem and emotional
status.
18
Some of the complications for bariatric surgery
- DVT, pulmonary Embolus, pneumonia, dumping
syndrome, loss of too much weight, injury to
pelvic organ, and leaks from a break in the
staple line, and death (1 nationwide).
19
Sign Consent
- The patient has the right to be informed of the
tests, treatments, or procedures, therefore,
should be asked to sign consent a legal piece of
paper that tells exactly what will be done to the
patient. Forms that gives caregivers permission
to certain tests, treatments, or procedures. If
unable to give his/her consent, someone who has
permission could sign the form instead.
20
Special Equipments
- With bariatric surgery patient, special
equipments have to be ordered and explained to
patients.
21
Post-operative Nursing Care
- By Stacy Moyston-Duckie
22
Complications developed after Bariatric surgery
- Bariatric-surgery patients are at risk for
developing complications related to surgery and
postoperative respiratory and gastrointestinal
disorders. - According to the International Bariatric surgery
registry, the leading cause of death following
bariatric surgery is pulmonary embolism,
anastomotic leaks and respiratory failure. - Other complications are wound infections,
incisional hernias, ulcers, bleeding,
constipation, cholelithiasis, dumping syndrome,
dehiscence, vitamin and nutrient deficiencies.
23
The role of the nurse in monitoring and managing
clients in postoperative
- Typically, during the postoperative recovery
period the nurse has to monitor and manage the
patient to reduce complications, by positioning
the patients head at least 30 degrees
semi-fowlers position to help breathing and by
reducing the weight of abdominal adipose tissue
pressing on the diaphragm. - Checking vital signs, assess for complications,
and provide skin and wound care, breathing
exercises using incentive spirometry. - Assess abdominal changes in appearance of volume
gastric or percutaneous drains, presence of
hematemesis or melena, and persistent cough.
These findings should be reported to the
physician for appropriate medical intervention.
(www.aafp.org). - Also encourage early ambulation to reduce the
risk of immobility.
24
Pain Medications
- Post-operative pain medications are given through
patient controlled analgesia (PCA) pump, which
dispenses (morphine) when the patient pushes a
button. They patient will also receive IV
injections of Torodol. - Torodol is similar to Motrin and helps relieve
abdominal muscle pain. After day two surgery the
patients medication will be switched from PCA
machine to a liquid medicine Roxicet liquid
Percocet that will be taken by mouth every 4-6
hours.
25
Appetite suppressant medications
- Appetite suppressants medications are given such
as Phentermine (Adepex-P, and Obsestin-30) which
acts directly on the appetite-control center in
the CNS to suppress and reduce hunger. - Sibutramine (Meridia), also reduces hunger and
increases sensations of satiety by inhibiting the
uptake of serotonin, norepinephrine, and dopamine
- Ursodiol, this drug is to taken twice a day, two
weeks after surgery. - Actigall is taken to prevent gallstones from
forming during rapid weight loss. Patients who
have done bariatric surgery will need to take
vitamin and mineral supplement for the rest of
their lives.
26
Preventive Measures Against Obesity
- Diet
- Exercise
- Group support
- by
- Na Pang
27
Exercise
- Exercise plays a crucial role after bariatric
surgery because - Promotes good circulation, respiration
- Increases metabolism, reduces adipose tissues
- How to start an effective exercise pattern
- Walking is the simple way to start the exercise
process - Then, try out different types of exercises to
find one that is enjoyable, running, treadmill. - However, exercises should be well-organized.
28
Ongoing Support
- Study shows that
- Support groups, one of the best things, after
bariatric surgery, keep the weight off. - Rationale
- Surgery requires lifestyle and behavioral
changes, patients need the support of family,
friends, and healthcare professionals to help
them get through any rough spots.
29
Nursing Care Plans for Bariatric Surgery
- by Marie Jimenez, SPN
30
- For patients undergoing bariatric surgery, it is
important to note that there are nursing care
plans designated for the preoperative and
postoperative phase.
31
Pre-op Nursing DiagnosisDisturbed
Self-Conceptrelated to obesity inability to
lose weight by conventional methods
Nursing Outcome Nursing Intervention Nursing Rationale
Client will demonstrate positive self-concept AEB Verbalizing feelings Positive statements Active participation in self-care Assess for signs and symptoms of a disturbed self-concept Implement measures to assist client to increase self-esteem Measures for client to adapt to body changes Recognition allows for prompt intervention An increase in self-esteem has a positive effect on client Impact of changes in self-concept
32
Post-op Nursing DiagnosisIneffective Breathing
Patternr/t increased RR associated with
fear/anxiety decreased RR associated with
depressant effect of anesthesia
Nursing Outcome Nursing Intervention Nursing Rationale
Client will maintain clear open airways AEB Normal breath sounds Normal rate depth of respirations Absence of dyspnea Assess for Signs Sx of an ineffective breathing pattern Monitor for i in oximetry results Place client in semi- to high fowlers position Instruct clients to use incentive spirometer q 1-2 h Recognition allows for prompt inter-vention Assist in evaluating respiratory status Allows for max. diaphragm excursion Promotes max. inhalation lung expansion
33
- Assessment provides vital clues regarding how
nursing care affects the psychosocial aspect of
the patient - Therapeutic communication encourages
self-awareness
- Nurses should be aware of protocols when
deviations of breathing patterns occur for proper
interventions to take place - Any signs of respiratory distress should be
reported and documented immediately
34
Discharge/Client teaching
- by
- Anaise E Ikama
35
Discharge/Client teaching
- Medications analgesics for pain, anti-emetics to
prevent dehydration and vitamins to ensure
adequate intake of nutrition - Wound care should be taught to prevent infections
- Activity progression any abdominal exercises,
weight - Lifting or swimming should not be attempted.
Ambulate to prevent DVT - Diet eat small meals due to the small size of
the stomach
36
Discharge/Client teaching
- Report symptoms
- To the ER
- Issues that require urgent medical attention,
such as chest pain, shortness of breath and
excessive - abdominal pain
- Contact the physician
- For non-emergent issues such as nausea,
vomiting, diarrhea or fever, redness, swelling,
drainage or bleeding from the incision
37
Discharge and Client Teaching
- byEdeneth Flores
38
D/C and Client teaching
- Instruct patients to take their prescribed
medications.
- Some of the medications are
- Analgesics ( pain)
- Anti-emetics (prevent dehydration)
- Vitamins ( to maintain the nutrition of the
patient)
39
D/C and Client teaching
- Teach wound care
- Teach about the S/S of infection
- Redness
- Swelling
- Pus/abnormal discharge from the incision site
- Pain
- Difficulty breathing
- Vomiting
- Fever
- Epigastric pain
- CALL MD if 2 or more of these symptoms persist
40
D/C and Client teaching NUTRITION
- Eat small snack due to small capacity of the
stomach. - Chew food slowly and cut into pieces.
- If able to tolerate liquids, the surgeon will
likely to recommend having a puree diet, then
begin eating 3 meals per day. - Eat a few tablespoons at a time to prevent the
stretching of the incision site.
- Eat a few tablespoons at a time to prevent the
stretching of the incision site - Includes protein to promote healing.
41
D/C and Client teaching
- Avoid heavy lifting
- Encourage ambulation and leg exercises
- Emphasize the importance of Follow-up visits
patients condition - Support groups