Skin Assessment PowerPoint PPT Presentation
1 / 31
Title: Skin Assessment
1
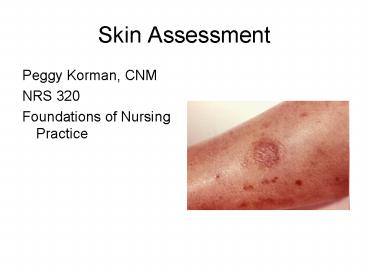
Skin Assessment
- Peggy Korman, CNM
- NRS 320
- Foundations of Nursing Practice
2
Integumentary System
- Nails
- Hair
- skin
3
Assessment Techniques
- Inspection
- Palpation
- Olafactory
4
Functions of the Skin
- Bodys External Protector
- Regulation of body temperature
- Sensory organ for pain, temperature, touch
5
Skin Assessment
- Normal skin color is consistent with genetic
background - Variations indicate some kind of problem
- It is important to identify probable causes for
skin to change its appearance - Skin is assessed for temperature, color,
moisture, turgor, texture
6
Skin Assessment
- Color normal skin color is consistent with
genetic background. Variations that indicate
problems include pallor, erythema, cyanosis and
jaundice - Document the patients color as
- Normal
- Pale
- Cyanotic
- Flushed
- jaundiced
7
What can cause these color changes?
- Pallor
- Eythema
- Jaundice
- Cyanosis
8
What can cause these color changes?
- Pallor anxiety, anemia
- Erythema carbon monoxide poisoning
- Jaundice cirrhosis
- Cyanosis hypoxemia
9
Assessing Dark-Skinned Patients
- No matter what a patients race or ethnicity, the
ability to note changes in skin color can mean
life or death. Assessment can be difficult or
inaccurate if you are unfamiliar with highly
pigmented skin tones.
10
Assessing Dark-Skinned Patients
- Adequate lighting-daylight is best
- Establish a baseline for skin tone by observing
least pigmented areas (palms, soles of feet,
buttocks, volar surfaceof forearm, mouth,
conjunctiva, nail beds) - Look for underlying reddish tone common to all
skin
11
Skin Temperature
- Temperature and other characteristics
- Warm and dry?
- Cool and clammy?
- Diaphoretic?
- Lesions? Wounds?
- Normal ASsessment
- Color normal, warm, dry and intact
12
What can cause these temperature changes?
- Generalized coolness
- Generalized warmth
- Localized coolness
- Localized hyperthermia
13
What can cause these temperature changes
- Generalized coolness Hypothermia or cool down
from OR - Generalized warmth Fever or increased metabolic
rate - Localized coolness Poor circulation in the area,
casts - Localized hyperthermia Infection, cut or surface
wound
14
Assessing Moisture
- Abnormal Skin Moisture
- Diaphoresis may accompany chest pain, fever,
anxiety - Dryness may present as dehydrated lips,
- or as dry or cracked mucus membranes
- Oiliness often causes acne
15
Assessing Texture
- Skin may be rough, dry, scaly, thick
- Skin may be very smooth, thin and moist (but not
necessarily oily) - Red, scaly patches may indicate eczema (in
infants may appear on cheeks or in diaper area) - Cradle cap manifests as greasy, yellow-brown
patchs on scalp when not properly washed
16
Thyroid conditions
- Hyperthyroidis Hypothyroidis
- smooth dry
- moist thick
- warm pale
- thin rough scaly
- itchy
17
Wound Assessment
- Wound
- Type incision,laceration, skin tear,
rash,perineal excoriation, decubitus - Appearance pink, red, eschar, sloughing,edematous
, ecchymosis - Dressing open to air, changed, sterile, dry,or
intact with sutures, staples, steristrips - Drainage serous, purulent, sanguinous, or none
18
Wounds with Eschar
19
Incisions
20
Bruising/Ecchymosis
- Ecchymosis should be consistent with reported
trauma. Bruising above the knees and below the
elbows is suspicioius and may indicate abuse. - Photograph ecchymosis (ED)
- The age of the ecchymosis can be determined by
color
21
Assessing Skin Turgor
- To determine turgor, pinch a fold of skin under
the clavicle or on the forearm so the top skin
separates from the underlying structure. Assess
as follows - Normal rises easily and returns to place
immediately - Abnormal skin does not return to place
immediately but exhibits tenting
22
Assessing Turgor
- Because poor skin turgor is more common and more
prominent in the elderly patient due to loss of
elasticity, check for skin turgor at the sternum. - Abnormal turgor is exhibited in dehydration,
edema, scleroderma, connective tissue disorders
23
Assessing Lesions
- Examine lesion color and elevation with a
flashlight - Wear gloves to examine lesions
- Record size (diameter) of lesions and surrounding
erythema in centimeters
24
Assessing Lesions
- Elevation
- Flat?
- Raised?
- Pedunculated (connected to the skin on a stem or
stalk-like base)
25
Assessing Lesions
- Distrubution Symmetrical or asymmetrical
distribution of lesions - Generalized (widely distributed)
- Localized
- Regional (specific to an area)
26
Assessing Pressure Ulcers
27
Stage One
- Intact skin with non-blanchable redness of a
localized area usually over a bony prominence
28
Stage Two
- The epidermis or topmost layer of the skin is
broken, creating a shallow open sore. Drainage
may or may not be present.
29
Stage Three
- Full thickness tissue loss. Subcutaneous fat may
be visible but muscle, bone and tendon are not
exposed. Slough may be present but does not
obscure the depth of the tissue loss. May
include undermining and tunneling.
30
Stage Four
- Full thickness skin loss with extensive
destruction, tissue necrosis, or damage to
muscle, bone, or supporting structures.
31
Assessing IV Site
- Note if IV is patent
- Note location and type of catheter
- Note if there is redness or edema
- Note if the dressing is dry and intact
- Note if IV site or dressing is changed