Skin -Normal Skin -Normal Stratified Squamous epithelial PowerPoint PPT Presentation
1 / 81
Title: Skin -Normal Skin -Normal Stratified Squamous epithelial
1
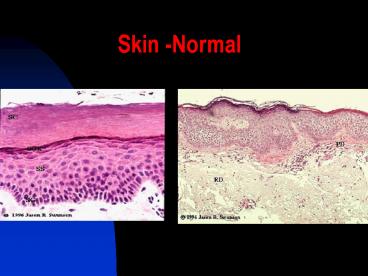
Skin -Normal
2
Skin -Normal
- Stratified Squamous epithelial cells
(keratinocytes) production of keratin protein, - Melanocytes production of a brown pigment
(melanin) - Langerhans cells take up and process antigens
- Neural end-organs and axonal processes
- Merkel cells
- within the basal cell layer
- mechanoreceptors or neuroendocrine function
3
Skin -Normal
- Sweat glands - temperature control
- Specialized dermal cells (dendrocytes) - for
antigen presentation as well as for production of
molecules (e.g., factor XIIIa) - Hair follicle- harbor protected repositories of
epithelial stem cells
4
Skin - Pathology
- DEFINITIONS OF MACROSCOPIC TERMS
- Macule
- Circumscribed lesion of up to 5 mm in diameter
characterized by flatness and usually
distinguished from surrounding skin by its
coloration. - Patch
- Circumscribed lesion of gt 5 mm in diameter
characterized by flatness and usually
distinguished from surrounding skin by its
coloration. - Papule
- Elevated dome-shaped or flat-topped lesion 5 mm
or less across. - Nodule
- Elevated lesion with spherical contour gt 5 mm
across.
5
Skin - Pathology
- Plaque
- Elevated flat-topped lesion, usually gt 5 mm
across (may be caused by coalescent papules). - Vesicle
- Fluid-filled raised lesion 5 mm or less across.
- Bulla
- Fluid-filled raised lesion gt 5 mm across.
- Blister
- Common term used for vesicle or bulla.
- Pustule
- Discrete, pus-filled, raised lesion.
- Wheal
- Itchy, transient, elevated lesion with variable
blanching and erythema formed as the result of
dermal edema.
6
Skin - Pathology
- Scale
- Dry, horny, plaque like excrescence usually the
result of imperfect cornification. - Lichenification
- Thickened and rough skin characterized by
prominent skin markings usually the result of
repeated rubbing in susceptible persons. - Excoriation
- Traumatic lesion characterized by breakage of the
epidermis, causing a raw linear area (i.e., a
deep scratch) often self-induced. - Onycholysis
- Separation of nail plate from nail bed.
7
Skin - Pathology
- Hyperkeratosis
- Thickening of the stratum corneum, often
qualitative abnormality of the keratin. - Parakeratosis
- Modes of keratinization characterized by the
retention of the nuclei in the stratum corneum. - Hypergranulosis
- Hyperplasia of the stratum granulosum, often due
to intense rubbing. - Acanthosis
- Diffuse epidermal hyperplasia.
- Papillomatosis
- Surface elevation caused by hyperplasia and
enlargement of contiguous dermal papillae.
8
Skin - Pathology
- Dyskeratosis
- Abnormal keratinization
- Acantholysis
- Loss of intercellular connections resulting in
loss of cohesion between keratinocytes. - Spongiosis
- Intercellular edema of the epidermis.
- Hydropic swelling (ballooning)
- Intracellular edema of keratinocytes, often seen
in viral infections. - Exocytosis
- Infiltration of the epidermis by inflammatory or
circulating blood cells. - Erosion
- Discontinuity of the skin exhibiting incomplete
loss of the epidermis
9
Skin - Pathology
- Ulceration
- Discontinuity of the skin exhibiting complete
loss of the epidermis and often of portions of
the dermis and even subcutaneous fat. - Vacuolization
- Formation of vacuoles within or adjacent to
cells often refers to basal cell-basement
membrane zone area. - Lentiginous
- Referring to a linear pattern of melanocyte
proliferation within the epidermal basal cell
layer. occur as a reactive change or as part of a
neoplasm of melanocytes.
10
Disorders of Pigmentation and Melanocytes
- 1.VITILIGO
- loss of pigment-producing melanocytes within the
epidermis - All ages and races, noticeable in darkly
pigmented individuals - Clinical lesions
- macules and patches of pigment loss
- Hands and wrists, axillae and perioral,
periorbital, and ano-genital skin (Muco-cutaneous
Jxns) - Koebnerization (as in Lichen planus)- lesions at
sites of repeated trauma - Morphology.
- Loss of melanocytes revealed by electron
microscopy - IHC for melanocyte-associated proteins (e.g.,
tyrosinase or Melan-A, or S-100
11
Disorders of Pigmentation and Melanocytes -
VITILIGO
- Pathogenesis.
- Theories
- 1) autoimmunity,
- 2) neurohumoral factors
- 3) self-destruction of melanocytes by toxic
intermediates of melanin synthesis - interesting facet of vitiligo -therapy with UVA
with use of the photosensitizing drug, psoralen
(known as PUVA) - Regain pigment initially at the ostia of hair
follicles, - Other causes of Hypopigmentation
- 1.Postinflammatory hypopigmentation
- 2.Albinism
- melanocytes are present but melanin pigment is
not produced - lack or defect in Tyrosinase
12
Disorders of Pigmentation and Melanocytes
- 2. FRECKLE (EPHELIS)
- MC pigmented lesions of childhood in lightly
pigmented individuals - after sun exposure
- Small (1 to several mm in diameter), tan-red or
light brown macules cyclic fashion with winter
and summer - DD from a Lentigo, which maintains stable
coloration independent of sun exposure. - Clinically
- hyperpigmentation -result of increased amounts
of melanin pigment within basal keratinocytes - melanocytes are normal in slightly enlarged
- café au lait spots are histologically
indistinguishable from freckles (evolve
independent from sun exposure)
13
Disorders of Pigmentation and Melanocytes
- 3.MELASMA
- mask-like zone of facial hyperpigmentation
- association with
- pregnancy "mask of pregnancy."
- oral contraceptives
- administration of Hydantoins,
- Idiopathic, resolves spontaneously
- poorly defined, blotchy, tan-brown macules and
patches involving the cheeks, temples, and
forehead bilaterally - Sunlight -accentuate
14
Disorders of Pigmentation and Melanocytes
- 4. LENTIGO (plural-lentigines)
- Hyperplasia of melanocytes often in infancy and
childhood - no sex or racial predilection
- Cause and pathogenesis - unknown.
- mucous membranes as well as the skin
- No change on exposure to sunlight.
- Essential histologic feature- hyperpigmented
basal cell layer - Elongation and thinning of the rete ridges
- variant - solar or actinic lentigo
- alteration in keratinocyte maturation in
sun-damaged skin of older pts. - Lentiginous -proliferation within the basal cell
layer in melanocytic tumor - Lentiginous nevi and melanomas (Acral lentiginous
melanomas).
15
Disorders of Pigmentation and Melanocytes
- 5.MELANOCYTIC NEVUS (PIGMENTED NEVUS, MOLE)
- (NEVI/ NEVUS benign lesion of the skin may be
pigmented or nonpigmented, flat or raised, smooth
or warty. May become malignant). - tan to brown, uniformly pigmented, small (usually
lt6 mm across), solid regions of relatively flat
(macules) to elevated skin (papules) with
well-defined, rounded borders - Morphology.
- formed by melanocytes grow in aggregates, or
"nests," along the dermoepidermal junction called
junctional nevi ? grow into the underlying dermis
as nests or cords of cells (compound nevi) ?older
lesions - intradermal - Maturation- correlates with enzymatic changes
(progressive loss of tyrosinase activity and
acquisition of cholinesterase activity - sequence of maturation - diagnostic importance in
distinguishing benign nevi from melanomas, which
usually show little or no maturation - Clinically, compound and dermal nevi are often
more elevated than junctional nevi
16
Disorders of Pigmentation and Melanocytes
- 6. DYSPLASTIC NEVI
- BK moles (initial two families studied)
- Clinically
- larger than most acquired nevi (often gt5 mm
across) - hundreds of lesions on the body surface
- flat macules, slightly raised plaques
- variability in pigmentation (variegation)
- borders that are irregular in contour
- occur on non-sun-exposed as well as on
sun-exposed body surfaces - in multiple members of families prone to the
development of malignant melanoma (the heritable
melanoma syndrome). - autosomal dominant
- peculiar linear fibrosis surrounding the
epidermal rete ridges
17
Disorders of Pigmentation and Melanocytes
- DYSPLASTIC NEVI
- Cytologic atypia ,irregular, often angulated,
nuclear contours and hyperchromasia - sparse lymphocytic infiltrate, loss of melanin
or melanin pigment incontinence - single nevus cells replace the normal basal cell
layer dermoepidermal junction, - lentiginous
hyperplasia - Precursors of malignant melanoma
- gt 5 of family members - melanoma
- probability of developing melanoma is 56 at age
59 years - Clark and associates
- steps? benign nevi ? aberrant differentiation ?
dysplastic ? metastasizing malignant tumors
18
7. MALIGNANT MELANOMA
- Skin, other sites (oral and anogenital mucosal
surfaces, esophagus, meninges eye) - Skin Mc site
- Non cutaneous UVEA of the eye
- Sunlight - important role
- Men - on upper back
- Women -both the back and legs
- Higher risk
- Carcinogens
- dysplastic nevus
- ( pre malignant ) gt 5 lt10mm
- hereditary factors
- Lightly pigmented individuals
- Clinical Features
- early feature itching ( itching moles bad)
- greater than 10 mm in diameter
- most important clinical sign -change in color,
size, or shape in a pigmented lesion - variations in pigmentation
- Borders not smooth, round, and uniform,
- If the size is more than 5mm follow
19
MALIGNANT MELANOMA
- Clinical warning signs
- 1) enlargement of a pre-existing mole,
- 2) itching or pain in a pre-existing mole,
- 3) development of a new pigmented lesion during
adult life, - 4) irregularity of the borders of a pigmented
lesion, and - 5) variegation of color within a pigmented lesion
- Growth Patterns and Morphology
- radial and vertical growth (longitudinal growth
into the epidermis, into blood vessels if more
than 1.7mm thick. Radial or horizontal not
important still limited to the dermis) - vertical component of growth
- clinically
- nodule in the relatively flat radial growth phase
- emergence of a clone of cells with true
metastatic potential ( moves from monoclonal to
multiclonal ) - probability of metastasis predicted by simply
measuring in millimeters the depth of invasion
below the granular cell layer
20
MALIGNANT MELANOMA
- Melanoma cells -
- larger than nevus cells
- large nuclei with irregular contours
- chromatin clumped at the periphery of the nuclear
membrane - large prominent red (eosinophilic) nucleoli
- nature and extent of the vertical growth phase
determine the biologic behavior of malignant
melanoma - Diagnostic Criteria and Prognostic Attributes
- assessment of prognosis based on
- 1) measurement of tumor depth in millimeters
- 2) number of tumor cell mitoses per square
millimeter in the microscope - 3) evidence of an immune response to the
superficial (radial) growth component (termed
regression) - 4) presence and degree of tumor infiltrating
lymphocytes (TILs) - 5) gender FEMALES GOOD
- (6) location
21
MALIGNANT MELANOMA
- More favorable prognosis
- tumor depth of less than 1.7 mm, (more than 1.7mm
bad prog.) - absence or low numbers of mitoses,
- presence of a brisk TIL tumor infultrating
lymphocytes response, - absence of regression,
- female gender, and
- location on extremity skin
- Gray zone - melanocytic tumors of uncertain
malignant potential (MELTUMP)
22
Benign Epithelial Tumors
- Derived from
- keratinizing stratified squamous epithelium of
the epidermis - hair follicles (keratinocytes)
- ductular epithelium of cutaneous glands
- confused with malignancy,
- Biopsy required
- 1. SEBORRHEIC KERATOSES
- arise spontaneously, on the trunk
- Face- Dermatosis papulosa nigra
- Clinically - round, flat, coin like waxy plaques
- uniformly tan to dark brown
- "stuck on" appearance easily peeled off.
- small, round, pore like ostia impacted with
keratin seen with a hand lens. (Differentiating
between malignant melanomas) - Part of paraneoplastic syndrome (Leser-Trélat
sign) - whorling" squamous cells resembling eddy currents
in a stream
23
2. ACANTHOSIS NIGRICANS
- Acanthosis proliferation hyperplasia of the
stratum spinosum of the epidermis - Hyperpigmented zones and "velvet-like" texture
- flexural areas
- cutaneous marker for associated benign and
malignant conditions - Benign type
- childhood or during puberty
- autosomal dominant
- with obesity or endocrine abnormalities (excess
cortico steroids) - pituitary and pineal tumors and with diabetes
- congenital syndromes
- Malignant type
- underlying GI adenocarcinoma.
24
3. FIBROEPITHELIAL POLYP
- squamous papilloma, skin tag
- Most common cutaneous lesions, during pregnancy
- part of a syndrome called Birt-Hogg-Dubé syndrome.
4. EPITHELIAL CYST (WEN)
- Invagination and cystic expansion of epidermis or
of the epithelium forming the hair follicle - filled with keratin and lipid-containing debris
- Histologic types
- Epidermal inclusion cyst
- Pilar or trichilemmal cysts
- Dermoid cyst (air follicles) budding outward from
its wall. - steatocystoma multiplex -resembling the sebaceous
gland duct
25
ADNEXAL (APPENDAGE) TUMORS
- Mendelian patterns of inheritance multiple
disfiguring - Eccrine poroma on the palms and soles derived
from eccrine sweat glands - Cylindroma on the forehead and scalp
- hat like growth turban tumor
- Syringomas, lesions of eccrine differentiation
- multiple, small lower eyelids
- Trichoepitheliomas, - follicular differentiation
- Markers for internal malignancy (trichilemmomas
and breast carcinoma of Cowden syndrome, also
seen in familial polyposis coli) cells try to
differentiate into hair follicles
26
KERATOACANTHOMA
- sun-exposed skin of whites older than age 50
years, facial skin - mimic squamous cell carcinoma (mutations in the
p53 gene) - heal spontaneously, without treatment
- flesh-colored, dome-shaped nodules
- central, keratin-filled plug, imparting a
crater-like topography - NB squamous cell carcinomas usually develop at a
site of chronic irritation
27
Premalignant and Malignant Epidermal Tumors
- ACTINIC KERATOSIS chronic exposure to sunlight
UVB ( sun light causes MCC in skin basal cell
carcinoma, best prognosis ,squamous cell
carcinoma, second best prognosis and malignant
melanomas, worse prognosis chronic exposure to
sunlight - excess keratin in lightly pigmented individuals.
- ionizing radiation, hydrocarbons, and arsenicals
- less than 1 cm in diameter are tan-brown, red,
or skin-colored - sandpaper-like consistency
- dyskeratosis with pink or reddish cytoplasm
- Dermis shows thickened, blue-gray elastic fibers
(elastosis), - nuclei in stratum corneum (parakeratosis)
- intercellular bridges are present
28
SQUAMOUS CELL CARCINOMA
- 2nd MC tumor arising on sun-exposed sites in
older people, - men gt women (Except for lesions on the lower
legs) - predisposing factors
- sunlight
- industrial carcinogens (tars and oils),
- chronic ulcers and
- draining osteomyelitis,
- old burn scars,
- ingestion of arsenicals,
- ionizing radiation,
- tobacco and betel nut chewing (in the oral
cavity).
Basal cell Carcinoma pallisding peripheral
cell Perpendicular to rest
29
SQUAMOUS CELL CARCINOMA
- exposure to UV light with subsequent DNA damage
- Immunosuppressed Drugs
- chemotherapy
- organ transplantation
- Xeroderma pigmentosum
- Sunlight has transient immunosuppressive effect
on - antigen-presenting Langerhans cells in the
epidermis - chemical agents- direct mutagenic effects by
producing DNA adducts - Morphology.
- less than 5 have metastases to regional nodes
30
BASAL CELL CARCINOMA
- Common, slow-growing ,rarely metastasize
- sites subject to chronic sun exposure
- in lightly pigmented people
- Immunosuppression
- defects in DNA repair (e.g., Xeroderma
pigmentosum - pearly papules often containing prominent,
dilated sub epidermal blood vessels
(telangiectasias) - unusually aggressive tumors- rodent ulcers
- resemble normal basal cell layer of the epidermis
- Two patterns
- multifocal growths originating from the epidermis
- nodular lesions growing downward deeply into the
dermis - islands of variably basophilic cells with
hyperchromatic nuclei surrounded by many
fibroblasts and lymphocytes - cells forming the periphery arranged radially
(pallisading)
31
Basal Cell Nevus Syndrome
- dominantly inherited
- numerous basal cell carcinomas in early life
- abnormalities of bone, nervous system, eyes, and
reproductive organs
32
MERKEL CELL CARCINOMA
- Merkel cell of the epidermis (neural
crest-derived cell) - for tactile sensation in lower animals
- clinically
- ulcerated nodules
- cytokeratin 20 positive
- capable of metastasis and are potentially lethal
- Fast metastasizing bad prognosis but rare
33
MOLECULAR GENETICS OF SKIN CANCERS
- organ constantly exposed to environmental hazards
most commonly affected by neoplasms - Basal cell carcinoma is the most common invasive
cancer in humans, - 1 million estimated cases per year in the United
States - incidence of malignant melanoma risen almost
exponentially - hereditary cancer syndromes provided important
insights of molecular pathogenesis of sporadic
nonmelanoma skin tumors and melanomas - basal cell nevus syndrome or Gorlin syndrome
- autosomal dominant
- multiple basal cell carcinomas - lt age 20
- other conditions
- tumors (especially Medulloblastoma a rapidly
growing tumor usually of the vermis of the
cerebellum, composed of preneurogliar cells and
ovarian Fibroma),
34
MOLECULAR GENETICS OF SKIN CANCERS
- pits of the palms and soles
- odontogenic keratocysts
- generalized overgrowth
- systemic manifestations
- intracranial calcification, cleft lip and palate,
abnormal segmentation of the vertebra, and rib
anomalies (bifid, fused, missing, splayed ribs) - Gene for NBCCS chromosome 9 (PTCH) (nevoid basal
cell carcinoma syndrome) - "two-hit" hypothesis
- born with a germ-line mutation
- second mutation either by environmental mutagens
or random genetic rearrangement - PTCH mutations in 30 of sporadic basal cell
carcinomas - Link- sun exposure and defects in PTCH and p53
- one-third have mutations (C to T transitions)
- Mutations in p53 occur in 40 to 60-60 of these
have UV signature - mutations in PTCH and p53 in Xeroderma
pigmentosum (90 and 40, bear the UV signature).
35
MOLECULAR GENETICS OF SKIN CANCERS
- Squamous Cell Carcinoma
- no inherited single gene defect associated with
squamous cell carcinomas - mutations in p53 in Caucasian patients with
actinic keratoses is high - Sunlight-alterations at the early stages of
carcinogenesis - pyrimidine dimers
- Unlike basal cell carcinomas, aneuploidy (
abnormal of chromosomes) is very common in
squamous cell carcinomas, loss of heterozygosity
of chromosomes 3, 9, and 17 occurs in
approximately 30 of cases - in severely immunosuppressed
- HPV types 5 and 8,
- pathogenesis of epidermodysplasia verruciformis
- formation of numerous cutaneous squamous cell
carcinomas
36
MOLECULAR GENETICS OF SKIN CANCERS
- Melanomas
- 10 to 15 arise in a familial setting
- familial melanoma syndrome (FMS)
- the familial BK mole syndrome
- have large numbers of dysplastic nevi
- is frequently deleted in melanomas
- main locus chromosome on 9p21and it encodes
p16INK4A - p16INK4A is the most commonly mutated gene in
familial melanoma - other genes CDK4 and BRAF
37
Tumors of the Dermis
- BENIGN FIBROUS HISTIOCYTOMA (DERMATOFIBROMA)
- family of benign dermal neoplasms of fibroblasts
and histiocytes. - adults and
- legs of young to middle-aged women
- Morphology
- Most common form -dermatofibroma
- benign, spindle-shaped fibroblasts arranged in a
well-defined, nonencapsulated mass within the
mid-dermis - overlying epidermal hyperplasia forms downward
elongation of hyperpigmented rete ridges ("dirty
fingers" pattern) - express coagulation factor XIIIa
38
Tumors of the Dermis
- DERMATOFIBROSARCOMA PROTUBERANS
- primary Fibrosarcoma of the skin.
- slow growing, locally aggressive, rarely
metastasize. - Clinically firm, solid nodules ,most frequently
on the trunk - Morphology
- In contrast to dermatofibroma, the overlying
epidermis is generally thinned - extension from the dermis into subcutaneous fat
(honeycomb" pattern) - composed of fibroblasts arranged radially,
reminiscent of blades of a pinwheel, a pattern
referred to as storiform - Mitoses not as numerous good prognosis
39
Tumors of the Dermis
- XANTHOMAS
- collections of foamy histiocytes within the
dermis lipid filled - Familial or acquired resulting in hyperlipidemia
- five types.
- Eruptive wax and wane according to variations in
plasma triglyceride and lipid contents - Tuberous and tendinous Achilles tendon extensor
tendons of the fingers - Plane with primary biliary cirrhosis
- Xanthelasma (without lipid abnormality) -eyelids.
40
Tumors of the Dermis
- DERMAL VASCULAR TUMORS
- Benign (capillary and cavernous hemangiomas),
- malformations (nevus flammeus or port-wine
stain), gone with age 14 to15 - malignant vascular tumors (Angiosarcomas) bad
prognosis seen in liver patients exposed to
plastics - angioproliferative lesions (Kaposi sarcoma HIV
(tumor like- bacillary angiomatosis)
41
Tumors of Cellular Immigrants to the Skin
- Primary cutaneous disorders
- Epidermal Langerhans cells- Langerhans cell
histiocytosis - T lymphocytes -cutaneous T-cell lymphoma (CTCL),
sezary syndrome - Dermal mast cells Mastocytosis
- See table in WBC review
42
Tumors of Cellular Immigrants to the Skin
- LANGERHANS CELL HISTIOCYTOSIS
- Histiocytosis X, multiple forms
- histologic patterns
- First-dermal infiltrate of large, round to ovoid
cells - second pattern -that resemble granulomas
- Third-xanthoma-like cytoplasm
- IHC methods -CD1a antigen
- ultrastructural identification of specific
organelles (Birbeck granules),
43
Tumors of Cellular Immigrants to the Skin
- MYCOSIS FUNGOIDES
- (CUTANEOUS T-CELL LYMPHOMA) ( seen in celiac
sprue and HTLV) - lymphoproliferative disorders affecting the skin
- Two different clinical types
- Mycosis fungoides, a chronic proliferative
process - Nodular eruptive variant, mycosis fungoides
d'emblée - Mycosis fungoides
- primarily in the skin and that may evolve into
generalized lymphoma - most commonly persons older than age 40.
44
Tumors of Cellular Immigrants to the Skin
- MYCOSIS FUNGOIDES
- (CUTANEOUS T-CELL LYMPHOMA)
- Clinically
- scaly, red-brown patches raised, scaling plaques
that may even be confused with psoriasis - Fungating nodules- Development of multiple
red-brown nodules correlates with systemic
spreading - seeding of the blood by malignant T cells is
accompanied by diffuse erythema and scaling of
the entire body surface (erythroderma), a
condition known as Sézary syndrome
45
Tumors of Cellular Immigrants to the Skin
- MYCOSIS FUNGOIDES
- (CUTANEOUS T-CELL LYMPHOMA)
- Morphology
- histological hallmark -Sézary-Lutzner cells they
have cerebriform nuclei ie looks like brain
(T-helper cells (CD4 positive) that
characteristically form band like aggregates
within the superficial dermis - infolded nuclear membranes -hyperconvoluted or
cerebriform contour - (epidermotropism) and form clusters Pautrier
microabscesses.
46
Tumors of Cellular Immigrants to the Skin
- MASTOCYTOSIS -? mast cells in the skin other
organs - Localized cutaneous form
- children and accounts for more than 50 of all
cases is termed urticaria pigmentosa - shortly after birth
- Systemic mastocytosis- 10
- adults
- prognosis may be poor
- Darier sign -localized area of dermal edema and
erythema (wheal) that occurs when lesion skin is
rubbed. - Dermatographism -area of dermal edema resembling
a hive that occurs in normal skin as a result of
localized stroking with a pointed instrument - Pathogenesis.-point mutation of the c-KIT
proto-oncogene
47
Disorders of Epidermal Maturation
- ICHTHYOSIS
- Hyperkeratosis-fishlike scales
- around the time of birth
- ichthyosis vulgaris (autosomal dominant or
acquired) - congenital ichthyosiform erythroderma (autosomal
recessive), - lamellar ichthyosis (autosomal recessive),
- X-linked ichthyosis.
- Acquired (noninherited) -in adults
- Associated with lymphoid and visceral malignant
neoplasms
48
ICHTHYOSIS
- Morphology
- compacted stratum corneum
- loss of the normal basket-weave pattern
- Pathogenesis
- primary abnormality -defective mechanisms of
desquamation - retention of abnormally formed scale
- adhesive organelles called Odland bodies, or
membrane-coating granules
49
Acute Inflammatory Dermatoses
- 1. URTICARIA
- characterized by
- localized mast cell degranulation
- dermal microvascular hyperpermeability
- pruritic edematous plaques called wheals
- Angioedema-deeper edema of both the dermis and
the subcutaneous fat - develop and fade within hours (usually lt24 hours)
or last for days or persist for months - superficial perivenular infiltrate of
mononuclear cells Eosinophils
50
URTICARIA
- Pathogenesis
- IgE-dependent degranulation can follow exposure
to a number of antigens - IgE-independent urticaria from substances
directly incite the degranulation of mast cells
(opiates, curare, and radiographic contrast
media) - Hereditary Angioneurotic edema- production of
vasoactive mediators (complement-mediated
urticaria). Deficiency complement 1 inhibitor
51
- 2. ACUTE ECZEMATOUS DERMATITIS
- Eczema
- Early lesion - red, papulovesicular less than
5mm, oozing, and crusted - Later - raised, scaling plaques
- acute spongiotic dermatitis
- chronic form - epidermal hyperplasia and
excessive scale - Clinical classification -allergic contact,
atopic, drug-related, primary irritant
photo-eczematous
52
. ACUTE ECZEMATOUS DERMATITIS
- Poison ivy- most obvious example is an acute
contact reaction - Edema
- in urticaria - localized to the perivascular
spaces of the superficial dermis - in spongiotic dermatitis - seeps into the
intercellular spaces of the epidermis, - Spongy like epidermis is due to prominent
Intercellular bridges - Intraepidermal vesicles are due to shearing of
intercellular attachment sites (desmosomes) and
cell membranes
53
ACUTE ECZEMATOUS DERMATITIS
- The pattern and composition of infiltrate give
clues to the underlying cause - systemic antigens (drugs) -lymphocytic
infiltrate, eosinophils, and extending deep as
well as superficial dermal vessels - surface contact with antigens -affects the more
superficial dermal layer
54
- 3. ERYTHEMA MULTIFORME
- hypersensitivity reaction to certain infections
and drugs - Infections-typhoid, and leprosy, herpes simplex,
mycoplasmal infections, histoplasmosis - drugs (sulfonamides, penicillin, barbiturates
- collagen vascular diseases (SLE, PAN,
dermatomyositis,). - malignant disease (carcinomas and lymphomas
55
3. ERYTHEMA MULTIFORME
- "multiform" lesions, including macules, papules,
vesicles, and bullae - symmetric involvement of the extremities
- extensive and
- toxic epidermal necrolysis -clinical situation
analogous to an extensive burn like a 3rd degree
burn - Stevens-Johnson syndrome seen in children
- symptomatic febrile form of the disease, result
in life-threatening sepsis ( sulfonamide use kids
causes) derm. Emergency - The target lesion exhibits central necrosis
surrounded by a rim of perivenular inflammation. - immunologic similarities
- fixed drug eruptions
- GVHD
- skin allograft rejection
56
Chronic Inflammatory Dermatoses
- 1. PSORIASIS
- 1 to 2 of people in the United States
- associated with arthritis, myopathy, enteropathy,
spondylitic joint disease, or the acquired
immunodeficiency syndrome - Clinically
- skin of the elbows, knees, scalp, lumbosacral
areas, intergluteal cleft, and glans penis. - Most typical lesion - salmon-colored plaque
covered by adherent scales (silver-white in color
) - Erythroderma-total body erythema
- Nail changes- separation of the nail plate from
the underlying bed (onycholysis), thickening, and
crumbling - pustular psoriasis-rare variant most dangerous
- generalized and life-threatening
57
2. SEBORRHEIC DERMATITIS
- More common than psoriasis
- Regions with a high density of sebaceous glands,
(scalp, forehead (especially the glabella),
external auditory canal, retroauricular area,
nasolabial folds) - Not a disease of the sebaceous glands
- Macules and papules with extensive scaling and
crusting - Fissures- behind the ears
- Dandruff is the common
- Infants-presents as cradle cap
- also be part of Leiner disease (with diarrhea and
failure to thrive) - severe and refeactory in HIV patients
58
2. SEBORRHEIC DERMATITIS
- Features
- both spongiotic dermatitis and psoriasis
- parakeratosis containing neutrophils and serum
are present at the ostia of hair follicles
(so-called follicular lipping) - HIV-apoptotic keratinocytes and plasma cells
- Etiology is unknown
- yeast Malassezia furfur with tinea versicolor
play a pivotal role (Rx.ketoconazole) - sebum is also involved
- patients with Parkinsonism show increased sebum
production increased incidence of seborrheic
dermatitis
59
3.LICHEN PLANUS
- "Pruritic, purple, polygonal papules"
- of the skin and mucous membranes
- self-limiting resolves spontaneously 1 to 2
years after onset - in chronic mucosal and para -mucosal
lesions-Malignant degeneration - zones of postinflammatory hyperpigmentation
- Wickham striae -papules are highlighted by white
dots or lines - zones of hypergranulosis
- loss of melanin pigmentation into the dermis as
the basal cell layer is destroyed
60
3.LICHEN PLANUS
- Multiple, symmetrically distributed on wrists and
elbows glans - 70 of cases, oral lesions are white, or netlike
areas - Koebner phenomenon
- infiltrate of lymphocytes along the
dermoepidermal junction - angulated zigzag
contour (saw- toothing) , - basal keratinocytes resemble of the stratum
spinosum (squamatization) also seen in vetaligo - Anucleate, necrotic basal cells inflamed
papillary dermis - colloid or Civatte bodies (also in any chronic
dermatitis) - epithelium of hair follicles is referred to as
lichen planopilaris. - pathogenesis -not known
- cell-mediated immune reactions
61
4. LUPUS ERYTHEMATOSUS
- SLE
- systemic manifestations,
- localized, cutaneous form -discoid lupus
erythematosus (DLE). - discoid lupus erythematosus (DLE).
- poorly defined malar erythema or erythematous
scaling plaques - develop or worsen with sun exposure
- keratotic plugs in follicular ostia
- lateral compression often produces wrinkling, a
sign of epidermal atrophy - lymphocytes along the dermoepidermal or the
dermal-follicular epithelial junction - Deep perivascular and periappendageal (e.g.,
around sweat glands) infiltrates
Band test
62
4. LUPUS ERYTHEMATOSUS
- infiltration of subcutaneous fat is called lupus
profundus. - basal cell layer -diffuse vacuolization
- epidermal layer -atrophied, with loss of the
normal rete ridge pattern - Involved hair follicles -epithelial atrophy,
dilated and plugged with keratin - Periodic acid-Schiff (PAS) -marked thickening of
the epidermal basement membrane zone - direct immunofluorescence - characteristic
granular band of immunoglobulin and complement
along the dermoepidermal and dermal-follicular
junctions ( lupus band test) - both lesional and normal skin in many cases of
SLE - seen in lesional skin but not normal skin in DLE
- Both formation and deposition of immune complexes
and complement components C5b to C9 -humoral
mechanisms of injury - In DLE band test positive only in affected skin
SLE both affected and normal skin
63
Blistering (Bullous) Diseases
- 1.PEMPHIGUS
- autoimmune blistering disorder resulting from
loss of the integrity of normal intercellular
attachments within the epidermis and mucosal
epithelium - life-threatening
- fourth to sixth decades of life
- 1) Pemphigus vulgaris -MC type (more than 80)
- mucosa and skin, especially on the scalp, face,
axilla, groin, trunk, - (2) Pemphigus vegetans -rare (groin, axillae, and
flexural surfaces) - presents not with blisters but with large, moist,
verrucous (wartlike), vegetating plaques, - (3) Pemphigus foliaceus -more benign form,
epidemic form in South America - (4) Pemphigus erythematosus rare, groin,
axillae, and flexural surfaces - face in a lupus erythematosus-like fashion.
- localized, less severe form of pemphigus foliaceus
64
1.PEMPHIGUS
- In all forms
- Acantholysis-dissolution, or lysis, of the
intercellular adhesion sites within a squamous
epithelial surface - Blister
- P. vulgaris - suprabasal acantholytic bliste
- P. foliaceus -selectively involves the
superficial epidermis at the level of the stratum
granulosum - Sera-antibodies (IgG) to intercellular cement
substance of skin and mucous membranes - Basis for direct and indirect diagnostic
immunofluorescence testing of skin and serum,
respectively - P. vulgaris antibody reacts with desmoglein 3
- P.foliaceus antibody reacts with desmoglein 1
65
2. BULLOUS PEMPHIGOID
- common autoimmune, vesiculobullous disease
- elderly
- less often
- involvement of mucosal surfaces
- bullae do not rupture as easily
- inner aspects of the thighs, flexor surfaces of
the forearms, axillae, groin, and lower abdomen - heal without scarring
- subepidermal, nonacantholytic blister
- Eosinophils showing degranulation
- beneath the epidermal basal cell layer.
- vacuolated basal cell layer
66
2. BULLOUS PEMPHIGOID
- subepidermal, nonacantholytic blister
- Eosinophils showing degranulation
- beneath the epidermal basal cell layer.
- vacuolated basal cell layer
- antibodies directed against proteins at the
dermal-epidermal junction. - linear zone deposition of immunoglobulin and
complement - lupus erythematosus is similar, but granular
- circulating antibody reacts with antigen
- (hemidesmosomes)
- Degranulating eosinophils are often associated
with necrosis of basal keratinocytes
67
3.DERMATITIS HERPETIFORMIS
- papules, vesicles, and occasional bullae on an
erythematous, often urticarial base - Malesgt Females
- third and fourth decades
- with celiac disease (both enteropathy respond to
a diet free of gluten) - plaques and vesicles are extremely pruritic
- bilaterally and symmetrically
- extensor surfaces, elbows, knees, upper back, and
buttocks grouped, name herpetiformis - early lesions
- Fibrin and neutrophils
- tips of dermal papillae, forming small
microabscesses subepidermal blister - Eosinophils of older lesions (creating confusion
with bullous pemphigoid)
68
3.DERMATITIS HERPETIFORMIS
- immunofluorescence
- granular deposits of IgA selectively localized in
the tips of dermal papillae - antibodies against gliadin, reticulin (IgA and
IgG ) - HLA-B8 and HLA-DRw3- prone
69
Immunofluorescence
pemphigus vulgaris
Bullous pemphigoid
Dermatitis herpetiformis
lupus band test
70
4. NONINFLAMMATORY BLISTERING DISEASES
EPIDERMOLYSIS BULLOSA, PORPHYRIA
- vesicles and bullae are not mediated by
inflammatory mechanisms. - Epidermolysis bullosa
- group of disorders with blisters at sites of
pressure, rubbing, or trauma, at or soon after
birth - Simplex type
- degeneration of the basal cell layer of the
epidermis - mutations in the genes encoding keratins 14 and 5
- Junctional type
- blisters in normal skin at lamina lucida
- scarring dystrophic types, blisters
- beneath the lamina densa,
- inherited disease
- mutations in the COL 7A1 gene that encodes type
VII collagen
71
NONINFLAMMATORY BLISTERING DISEASES
EPIDERMOLYSIS BULLOSA, PORPHYRIA
- Porphyria
- inborn or acquired disturbances of porphyrin
metabolism - Classification based on clinical and biochemical
features - five major types
- Cutaneous
- urticaria and vesicles that heal with scarring
- exacerbated by exposure to sunlight
- subepidermal vesicle
- marked thickening of the walls of superficial
dermal vessels
72
Disorders of Epidermal Appendages
- ACNE VULGARIS
- middle to years late teenage males have more
severe disease - milder in Asian descent
- in adolescents result of physiologic hormonal
variations and alterations in hair follicle
maturation - induced or exacerbated by drugs
- occupational contactants
- Some families
- heavy clothing and tropical climates
- noninflammatory and inflammatory types
- without a visible central plug
- Open comedones
- central black keratin plug
- oxidation of melanin pigment (not dirt)
- Closed comedones
- open and closed comedones
73
ACNE VULGARIS
- Four key components
- changes in keratinization of follicular
infundibulum - increase in size of sebaceous glands with puberty
or increased activity - lipase-synthesizing bacteria (Propionibacterium
acnes) - induction of inflammation in the follicle
- Dermal abscesses with scarring
- Pathogenesis is incompletely understood
- Endocrine (especially androgens)
- bacterial lipases of Propionibacterium acnes
- resulting in the earliest inflammatory phases
- clinical improvement with synthetic vitamin A
derivative 13-cis-retinoic acid (isotretinoin)
74
Panniculitis
- ERYTHEMA NODOSUM MCC ERYTHEMA
- INDURATUM
- Panniculitis
- inflammatory reaction in the subcutaneous fat
- Erythema nodosum
- the most common form of panniculitis
- acute presentation in infections (beta-hemolytic
streptococcal infection, tuberculosis and, less
commonly, coccidioidomycosis, histoplasmosis, and
leprosy - drug (sulfonamides, oral contraceptives),
sarcoidosis, inflammatory bowel disease) - malignant neoplasms
- lower legs
- erythematous plaques and nodules
- better felt than seen
- Biopsy usually required
75
Panniculitis
- Erythema induratum
- uncommon type of panniculitis
- adolescents and menopausal women
- cause is not known
- primary vasculitis affecting deep vessels
- most commonly occurs without an associated
underlying disease. - Erythema nodosum
- Vasculitis is not present
- erythema induratum,
- necrotizing vasculitis
- granulomatous inflammation and zones of caseous
necrosis - Weber-Christian disease (relapsing febrile
nodular panniculitis) is a rare form of lobular,
nonvasculitic panniculitis seen in children and
adults - Factitial panniculitis caused by self-inflicted
trauma or injection of foreign or toxic substances
76
Infection and Infestation
- 1. VERRUCAE (WARTS)
- common lesions of children and adolescents
- caused by HPV, self-limited, regressing
spontaneously - Classification
- Verruca vulgaris is the most common type of wart
- hands, dorsal surfaces and periungual areas
- Verruca plana, or flat wart- face or the dorsal
- hands
- Verruca plantaris and verruca palmaris -soles and
palms - Condyloma acuminatum (venereal wart) occurs on
the penis, female genitalia, urethra, perianal
areas, and rectum - cytoplasmic vacuolization (koilocytosis)
- verrucous or papillomatous epidermal hyperplasia
77
2. MOLLUSCUM CONTAGIOSUM
- common, self-limited viral disease of the skin
caused by a poxvirus - brick shaped,
- largest pathogenic poxvirus in humans
- largest viruses in nature
- children and young adults
- trunk and anogenital areas
- Firm, pruritic, pink to skin-colored umbilicated
papules - curd-like material on staining with Giemsa show
diagnostic molluscum bodies - cytoplasmic inclusion in cells of the stratum
granulosum and the stratum corneum - virions are present within molluscum bodies.
78
3. IMPETIGO
- Common superficial bacterial infection of the
skin - Highly contagious - healthy children, adults in
poor health - impetigo contagiosa and impetigo bullosa (differ
in size of the pustules) - Staphylococcus aureus
- Face and hands
- Honey-colored crust.
- characteristic microscopic features
- accumulation of neutrophils beneath the stratum
corneum - Sub-corneal pustule
- Blister formation - due to bacterial production
of a toxin specifically cleaves the desmoglein 1
cell-to-cell adhesion within the uppermost
epidermis
79
4. SUPERFICIAL FUNGAL INFECTIONS
- confined to the stratum corneum
- caused primarily by dermatophytes
- organisms grow in the soil and on animals
- Tinea capitis usually occurs in children
- Scalp-asymptomatic, often hairless patches of
skin - erythema, crust formation, and scale
- Tinea barbae - uncommon disorder beard area of
adult men - Tinea corporis - common superficial fungal
infection of children affecting body surface
80
4. SUPERFICIAL FUNGAL INFECTIONS
- Tinea cruris - inguinal areas of obese men during
warm weather - Tinea pedis (athlete's foot) affects 30 to 40
of the population - diffuse erythema and scaling of web spaces
- Spread to nails- onychomycosis.
- Tinea versicolor - upper trunk
- Caused by Malassezia furfur, a yeast
- present in cornified layer of lesional skin,
hair, or nails - scraping - produce colonies
- Fungal cell walls, rich in MPS, stain bright pink
to red with PAS stain
81
5 . ARTHROPOD BITES, STINGS, AND INFESTATIONS
- Arachnida (spiders, scorpions, ticks, and mites),
Insecta (lice, bedbugs, bees, wasps, fleas,
flies, and mosquitoes), and Chilopoda
(centipedes) - Vectors for secondary invaders, such as viruses,
bacteria, rickettsiae, and parasites - Black widow spider venom -severe cramps and
excruciating pain - Brown recluse spider venom - enzymes that produce
tissue necrosis